Pain Management and Chronic Pain Care
Led by brain and pain specialist in Tampa, focused on identifying what is truly driving your pain.
Some people come to us because pain started after an injury. Others come because pain has lasted longer than it should, or keeps returning even after treatment.
When symptoms do not clearly match imaging, or relief never lasts, it is often a sign the full picture has not been evaluated. Care here begins with a thorough medical exam and a clear explanation of what is driving the problem, then the right next step is recommended based on findings, not assumptions.
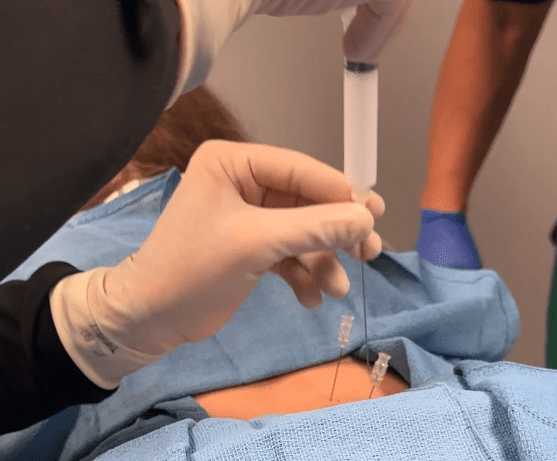
“I’m incredibly grateful for the care that Dr. Gleis has provided for my neck and back pain. His customized treatment plan, including targeted injections, has greatly improved my quality of life. He is compassionate and attentive, always taking time to listen and explain each step.”
-Douglas S.

Who Is Dr. Christopher Gleis, MD
Dr. Christopher Gleis is a board certified physician who leads pain management at Genesis Brain Institute. He is one of the few pain management specialists also board certified in anesthesiology, which gives him advanced training in nerve pathways, pain signaling, and full body evaluation.
Patients often come to Dr. Gleis after pain has persisted, shifted, or returned despite treatment. His approach starts with a thorough medical exam and clinical correlation, then a plan guided by findings, not routine.
Common Pain Problems We Evaluate and Treat
These are common reasons patients seek pain management and chronic pain care at Genesis Brain Institute in Tampa.
- Neck pain
- Back pain
- Shoulder pain
- Knee pain
- Joint pain
- Sciatica
- Numbness and tingling
- Headaches
- Acute pain after injury
- Unresolved chronic pain
Pain can be complex. Evaluation focuses on identifying what is truly driving symptoms before deciding what makes sense next.
Common Pain Problems We Evaluate and Treat
Pain is not always as simple as one spot, one scan, one solution.
Sometimes pain is tied to a clear injury or flare. Other times it persists for months, shifts locations, or keeps returning even after treatment. When that happens, it usually means the underlying driver has not been fully identified, or the nervous system is still stuck in a protective pattern.
Pain management here starts by clarifying what type of pain you are dealing with and what is most likely driving it.

Acute Pain vs Chronic Pain
Acute pain is often connected to a recent event, such as a strain, accident, or sudden flare. The focus is on evaluation, stability, and protecting recovery.
Chronic pain is different. When pain lasts longer than expected or keeps returning, it often involves multiple drivers, such as joints, discs, nerves, muscular compensation, inflammation, or nervous system signaling.
The goal is not to label pain quickly. The goal is to understand it correctly.
A Diagnostic Approach Driven by Medical Judgment, Not Automation
Rather than treating an MRI report in isolation, Dr. Gleis begins with a thorough medical exam and clinical correlation.
Symptoms, movement patterns, neurological findings, and imaging are evaluated together. When these elements do not align, that mismatch becomes a clue, not something to ignore.
This is how the true source of pain is identified, and why treatment decisions are guided by findings and response, not preset sequences.
How Patients Move Through Pain Management at
Genesis Brain Institute in Tampa
Pain management works best when the plan is based on what is actually happening, not what someone assumes is happening. That is why care with Dr. Gleis follows a clear process, guided by medical judgment, not automatic sequences.
Step 1: A Thorough Evaluation
The first step is a detailed medical history and conversation about your symptoms.
This includes how pain started, what makes it better or worse, how it affects sleep and function, and what has already been tried. If you have had prior care, that context matters. If you have had imaging, reports, or procedures, those details matter too. This is where patterns often begin to show up.
Step 2: A Real Physical Exam and Clinical Correlation
A hands-on physical exam is a core part of care.
Dr. Gleis looks at movement patterns, strength, sensation, reflexes, and pain behavior. Findings are then compared with symptoms and imaging when available. If imaging does not match what you are experiencing, that mismatch becomes meaningful. It often explains why prior treatment did not hold.

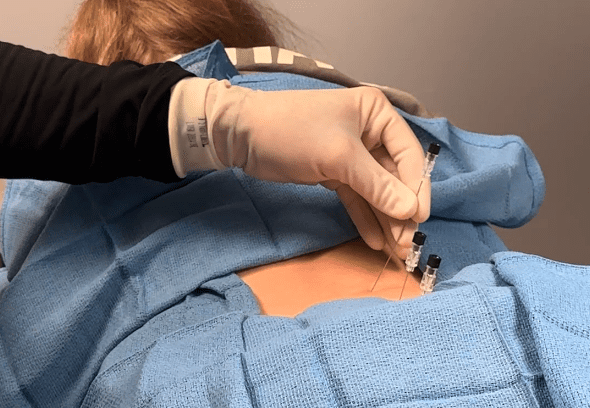
Step 3: A Plan Built Around the True Driver of Pain
After evaluation and examination, the goal is clarity.
For some patients, the right next step is conservative care and monitoring. For others, it may involve additional evaluation, coordination with other providers, or targeted treatment options based on the findings.
As a brain and pain specialist, Dr. Gleis considers structural drivers and nervous system related drivers together, especially when pain has become persistent or difficult to explain. The plan is not one size fits all. It is based on what is most likely driving symptoms.
Step 4: Reassessment Based on Response
Pain management should evolve as the clinical picture becomes clearer. If something helps, it is built upon. If something does not help, it is reassessed, not repeated out of routine.
This protects patients from cycling through the same steps without progress and keeps care grounded in response, function, and medical judgment.
What to Bring to Your Appointment
If available, bring:
- Imaging discs and reports, MRI, CT, X ray
- A list of medications and supplements
- Prior procedure history, if applicable
- Any relevant records from previous providers
If you do not have these, do not let that stop you. The goal is still to begin with a clear evaluation.
When Interventional Pain Management Makes Sense
Interventional pain management is not the first step for every patient. It is one tool that may be appropriate when the evaluation supports it and conservative care has not been enough.
As a brain and pain specialist, Dr. Gleis looks at the full pattern first. Symptoms, physical exam findings, and imaging are reviewed together so the decision is guided by medical judgment, not routine.


Consider Interventional Pain Management when:
- You have already tried conservative care such as physical therapy and supportive medication options, and symptoms are not improving
- Pain is limiting function, sleep, or daily activity and the clinical findings support a targeted approach
- Imaging and examination suggest inflammation or irritation involving joints, discs, or nerves
- You have already completed conservative care through a primary care provider, chiropractor, or previous pain treatment, and the issue has become persistent
What Interventional Pain Management can Include
Depending on the clinical picture, Dr. Gleis may discuss options such as:
Facet joint injections
Epidural injections
Nerve blocks
Radiofrequency Ablation
SI joint injections
How the decision is made
Pain Management FAQ
What does a brain and pain specialist mean
Do you treat chronic pain in Tampa
What types of pain do you treat
Common reasons patients come include neck pain, back pain, joint pain, shoulder pain, knee pain, sciatica, numbness and tingling, headaches, acute pain after injury, and unresolved chronic pain.
Do you prescribe pain medication
Medication may be considered when appropriate, but it is not the foundation of care. Long term reliance on narcotics is avoided whenever possible, with a focus on identifying and addressing what is driving symptoms.
Are injections always part of pain management
No. Interventional pain management is not automatic with Dr. Chris Gleis. Options are discussed only when the evaluation supports it and when conservative steps have not been enough.
When does interventional pain management make sense
It may be considered when pain is significantly limiting function, sleep, or daily activity and conservative care has not improved symptoms, often after a course of physical therapy. It can also be appropriate sooner when conservative care has already been tried elsewhere.
What if my MRI is normal but I still have pain
Imaging is one tool. When symptoms do not match imaging, the physical exam and clinical correlation become especially important. That mismatch can help clarify what may be getting missed.
What if I have already tried pain treatment elsewhere
That is common. Prior records and response to treatment are reviewed carefully. If something did not help, repeating it is not assumed to be the answer.
How do you decide if pain is coming from a nerve, joint, or disc
This is determined through a combination of history, physical examination, symptom patterns, and imaging review when available. The goal is to identify the most likely pain generator before selecting any intervention.
What should I bring to my appointment
If available, bring imaging discs and reports, a medication list, prior procedure history, and any relevant records from previous providers. If you do not have these, you can still begin with a thorough evaluation.
Do you see patients who travel for care
Yes. Genesis Brain Institute is located near Tampa International Airport in the Rocky Point area. Our office park has on site hotel options, including the Westin and DoubleTree by Hilton, making travel simple for patients visiting from outside the area.
How do I schedule an evaluation
Patients may schedule directly with Genesis Brain Institute to begin a medical evaluation with Dr. Christopher Gleis.
What Patients Are Saying
ED RIOS

Chloe Derian

Douglas S

Cecelia Cosgrove

Mary Barnard

Darlene Kalada

Tara Dowd
Dr Gleis is kind and patient with everyone. He listens and explains everything so you feel comfortable.His staff is friendly and it’s a pleasant environment. He helped my husband with his shoulder pain and we truly appreciate his professionalism.

Felix

