Post concussion syndrome treatment in Tampa is often overlooked until daily life starts to change.
After a car accident, many people assume that if they are able to go home the same day, the injury must be minor. What they do not realize is that concussion symptoms, nervous system disruption, and emotional changes often emerge gradually as pain persists and routines become harder to maintain.
Fortunately, in the case you are about to learn from, action was taken early. Rather than waiting to see if symptoms would resolve on their own, the patient underwent a comprehensive evaluation and was followed over time using objective diagnostics and clinical interviews. That early decision created clarity and allowed treatment to evolve as symptoms changed.
In this article, you will learn why simply getting checked out after an accident matters, even when you are unsure if something is wrong.
More importantly, you will learn how early diagnostics and targeted treatment changed the course of recovery in this mTBI case.
Specifically, you will learn:
- How advanced diagnostics, including qEEG brain mapping and clinical interviews, helped identify concussion related brain dysfunction alongside confirmed spinal injuries
- How treatment was adjusted as symptoms evolved, including addressing depression that developed after the patient could no longer train or work in a fitness environment
- How therapies such as Transcranial Magnetic Stimulation (TMS treatment) and additional Hyperbaric Oxygen Therapy (HBOT) were used to support brain function, mood regulation, and recovery over time
Many people hesitate to seek care after an accident because they worry about cost or pressure from insurance companies to settle quickly.
In many motor vehicle accidents, medical benefits are available specifically to cover evaluation and treatment early, before symptoms fully declare themselves. We explain this in more detail in our related article on brain injuries in car accidents, which is linked here if you want additional context.
In the case you are about to learn from, the accident occurred when the patient slowed for a changing light and was struck by a vehicle pulling a heavy trailer that accelerated to beat the light.
The impact was severe enough to total the vehicle, throw it across the intersection, and shatter the rear windshield.
Although the patient returned home that day, stiffness, neck pain, back pain, vision problems and headaches developed by the following morning and continued to worsen rather than resolve.

Further evaluation confirmed that the injuries were significant. Imaging revealed multiple herniated discs in the cervical and lumbar spine, confirming that the body had absorbed substantial force during the collision. At the same time, changes in focus, energy, and emotional regulation began to appear, pointing to post concussion syndrome rather than an isolated orthopedic injury.
As weeks passed, the neurological impact became harder to ignore. The patient had previously trained at the gym daily for two to three hours daily, worked in a fitness environment, and planned a future career in the field. When pain and neurological strain made that level of activity impossible, depression developed, not as a preexisting condition, but as a direct consequence of injury and loss of identity.
This story is not about injury alone. It is about what happens when diagnostics guide mTBI treatment and how progress is measured over time.
By using pre and post evaluations and adjusting care to include therapies such as TMS treatment out of the Tampa office of Genesis Brain Institute and additional Hyperbaric Oxygen Therapy, recovery became something that could be supported, tracked, and improved rather than guessed.
Why Post Concussion Symptoms Can Worsen Days or Weeks After an Accident
In her follow-up conversations, Dr. Emily explained that concussion symptoms often change over time because the brain can initially compensate after injury. Early on, the brain may continue to function well enough to get through daily life, especially in individuals who are active, motivated, or high functioning. As those compensatory patterns wear down, symptoms that were not obvious at first can become more noticeable.
She also emphasized that many concussion related issues only become apparent when the brain is asked to perform under normal demands again. When physical activity, work, or stress increases, the brain may struggle to regulate efficiently, leading to fatigue, headaches, emotional changes, or difficulty maintaining focus. These changes are not sudden injuries, but signs that the brain is working harder than it should.
Dr. Emily noted that this is why concussion symptoms are often confusing for patients and families.
Structural imaging can identify injuries like herniated discs, but it does not show how well the brain is functioning. Functional changes in brain activity can evolve as the nervous system responds to pain, inflammation, and ongoing stress.
In this case, the progression of symptoms aligned with what Dr. Emily commonly sees after a concussion.
Delayed symptoms did not indicate a new injury, but rather revealed areas of brain strain as recovery unfolded. This is why she stresses early evaluation and continued monitoring, so care can be guided by how the brain is actually functioning over time.
How a Brain Injury and Spinal Injury Interact After a Car Accident
Dr. Gleis explained that car accidents often transmit force through the spine in ways that are not immediately obvious.
Even when people are focused on the impact to the head, the neck and lower back frequently absorb significant mechanical stress, leading to joint irritation, inflammation, and nerve involvement. These spinal injuries can continue sending distress signals to the brain long after the initial trauma.
Dr. Emily emphasized that the brain and spine do not operate as separate systems. When spinal joints and surrounding nerves are irritated, they continuously communicate with the brain, increasing overall nervous system load.
This ongoing input can make it harder for the brain to regulate mood, focus, sleep, and stress, especially after a concussion.
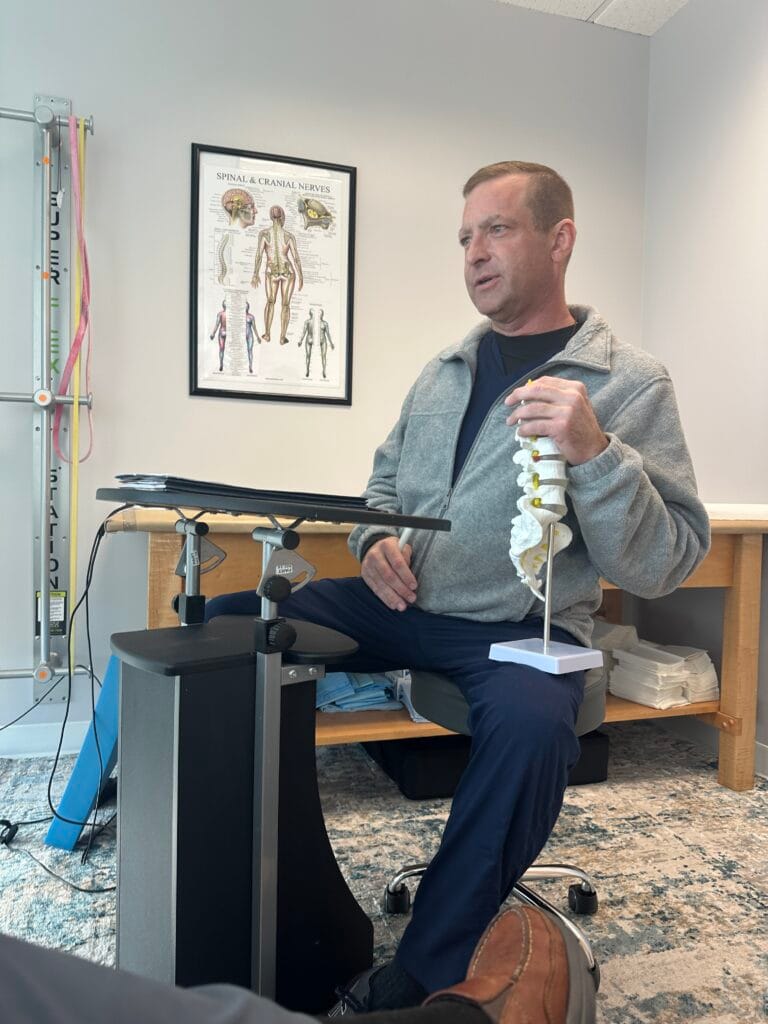
In this case, imaging confirmed multiple herniated discs, validating the physical source of pain Dr. Gleis identified during examination. However, the presence of structural injury did not fully explain the cognitive and emotional symptoms that followed. Dr. Emily noted that when the brain is already recovering from a concussion, persistent pain signals from the spine can amplify neurological strain.
Both clinicians stressed that unresolved spinal pain can slow neurological recovery. The brain must constantly process incoming pain signals, reducing its capacity to heal and self regulate. This interaction helps explain why treating only the spine or only the brain often leads to incomplete recovery.
By addressing spinal injury and brain function together, care becomes more coordinated and effective. Dr. Gleis focused on reducing pain and nerve irritation, while Dr. Emily evaluated how the brain and nervous system were responding over time. This combined approach helped reduce competing stressors on the nervous system and created a more stable environment for recovery.
The Role of Advanced Diagnostics in Post Concussion Syndrome Treatment
Dr. Emily explained that symptoms alone are not enough to understand what is happening after a concussion. Many patients can describe how they feel, but without objective data, it is difficult to know which parts of the brain are struggling and why symptoms are changing over time. This is why advanced diagnostics are used early, not to label a condition, but to understand brain function.
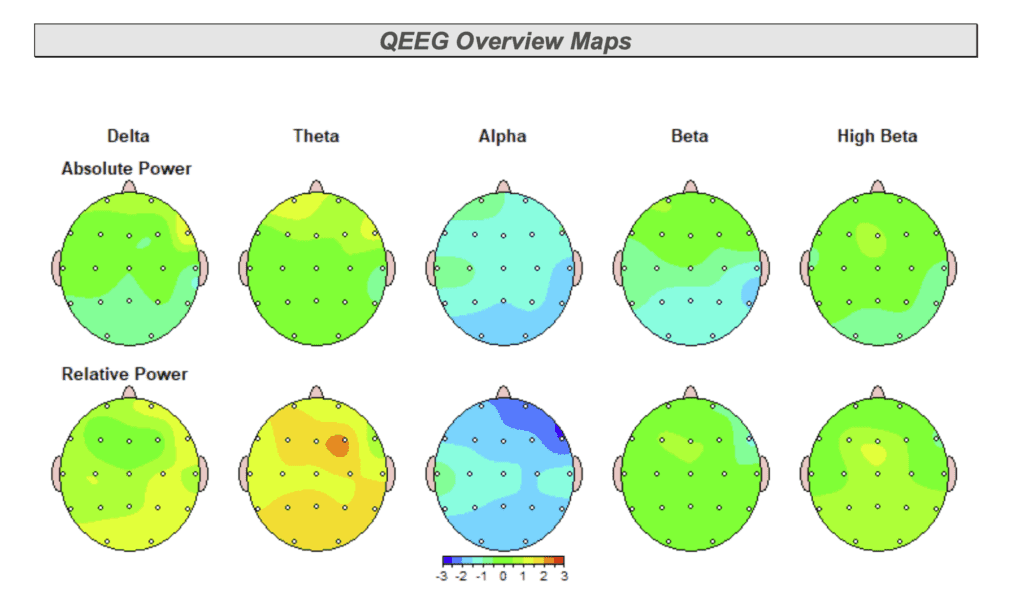
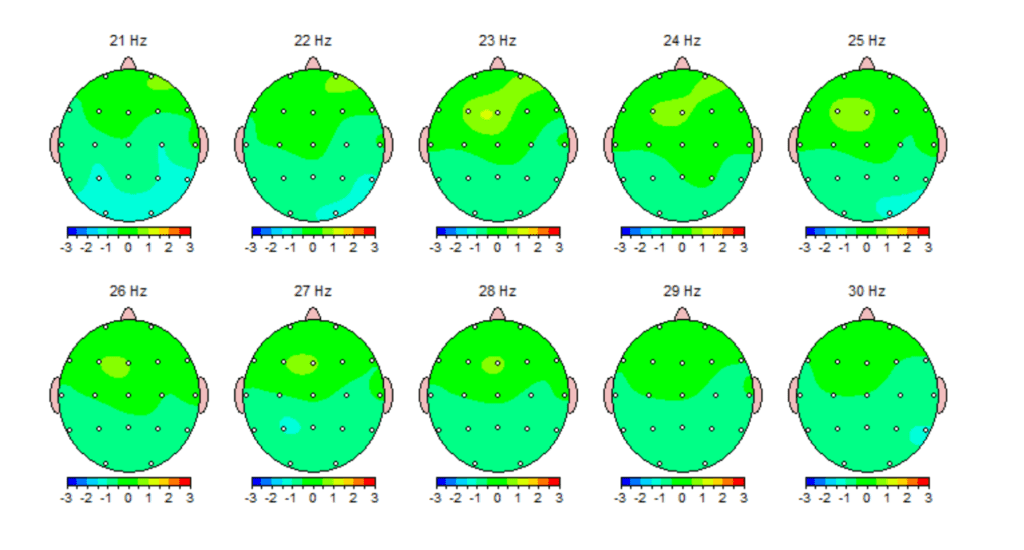
In this case, qEEG brain mapping was used to evaluate how different regions of the brain were communicating and regulating activity. Dr. Emily emphasized that a qEEG does not diagnose a concussion on its own, but provides insight into how the brain is functioning compared to expected patterns. These findings helped explain symptoms such as mental fatigue, reduced stress tolerance, and difficulty maintaining regulation.
She also highlighted the importance of pairing diagnostic data with clinical interviews.
Understanding how the patient’s daily life, stress levels, pain, and activity tolerance were changing provided essential context for interpreting the brain data. The combination of objective findings and patient experience allowed care to be individualized rather than protocol driven.
Most importantly, these diagnostics established a baseline. Dr. Emily explained that having a clear starting point makes it possible to measure progress and adjust treatment as the brain responds. Without this baseline, changes can be missed, misunderstood, or dismissed, especially when symptoms fluctuate during recovery.
What the Initial Brain Evaluation Revealed after the qEEG Brain Mapping
During the initial evaluation, Dr. Emily focused on understanding how the patient’s brain and nervous system were functioning after the accident, not just how symptoms were being described. She explained that concussion related issues often involve regulation, processing speed, and communication between brain regions, which cannot be seen on structural imaging alone. The goal of the evaluation was to identify where the brain was under strain and how the nervous system was responding overall.
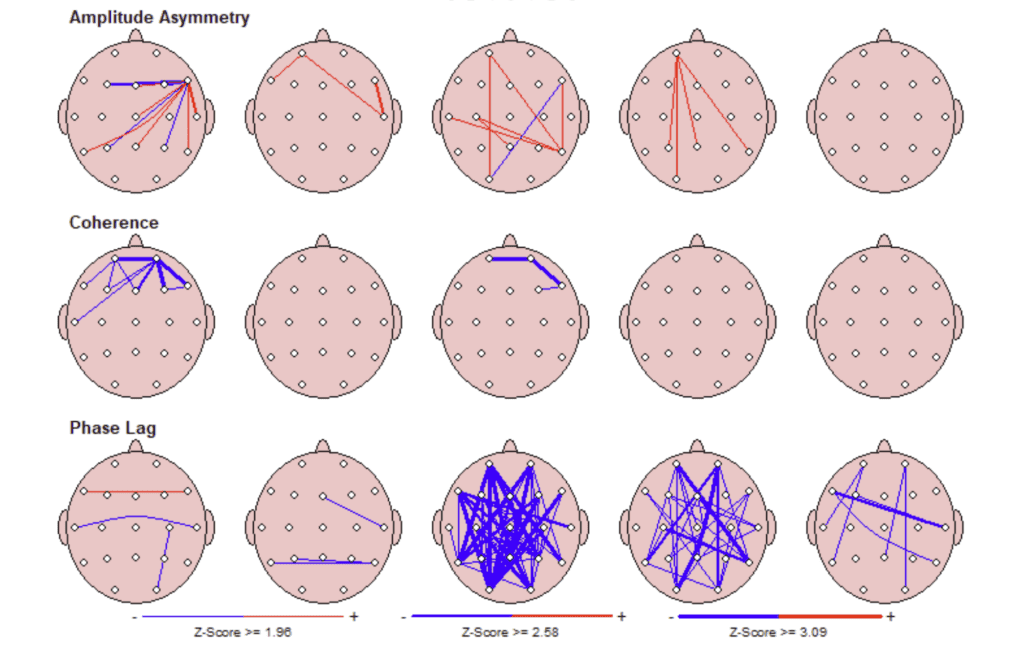
qEEG brain mapping was used as one part of this process to assess patterns of brain activity. Dr. Emily reviewed how certain regions were working harder than expected while others were not regulating efficiently. These findings helped explain why the patient experienced mental fatigue, difficulty tolerating stress, and changes in focus as daily demands increased.
Additional functional assessments, including balance testing and pupil response testing and cognitive testing, provided further insight into nervous system regulation.
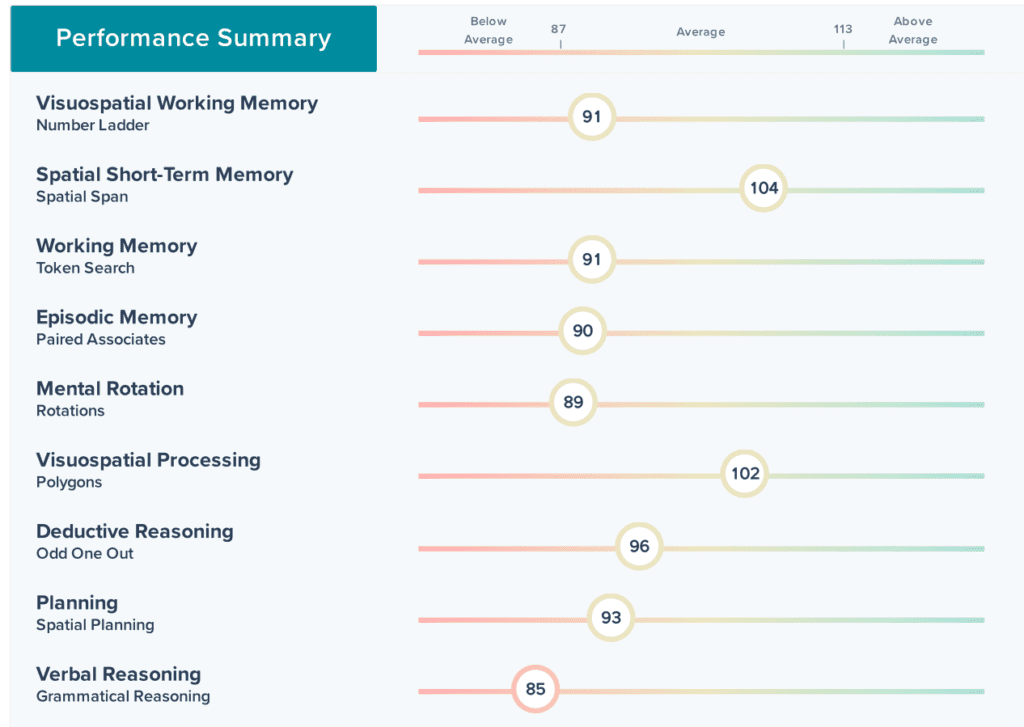
Dr. Emily explained that these measures help show how well the brain is integrating sensory input and maintaining stability after injury. When combined with the qEEG brain mapping data and clinical interview, they helped form a clearer picture of how the concussion was affecting the patient beyond pain alone.
Importantly, these findings did not exist in isolation. Dr. Emily emphasized that the results needed to be interpreted in the context of ongoing spinal pain, reduced physical activity, and daily stress. This comprehensive view allowed mTBI treatment to be tailored to what the brain and nervous system actually needed, rather than following a standard protocol.
Coping With PTSD After a Car Accident: When Depression Becomes Part of Recovery
Dr. Emily explained that after a car accident, symptoms associated with PTSD and depression often overlap rather than occur in isolation. When the nervous system remains in a heightened state following trauma, the brain can struggle to return to normal regulation. Over time, this ongoing stress response can contribute to emotional changes, including depression.
In this case, the patient experienced continued nervous system strain as physical pain persisted and normal routines were disrupted. The inability to exercise, combined with ongoing symptoms, created a constant signal of stress to the brain. Dr. Emily noted that when the brain stays in a survival oriented state, emotional regulation and mood stability can decline.
She also explained that PTSD related responses do not always present as fear or panic alone. They can appear as emotional flattening, low motivation, or a loss of interest in activities that once provided structure and purpose. When these patterns occur alongside concussion related brain dysfunction, depression can emerge as part of the injury process rather than as a separate mental health condition.
Because of this progression, Dr. Emily referred the patient to Dr. Craig Jorden Jr., who works within the clinic to support patients with neurological and mood related symptoms. After evaluation, Transcranial Magnetic Stimulation was prescribed as a non medication option to support mood regulation and brain function during recovery.
Dr. Emily emphasized that addressing depression without supporting the underlying brain and nervous system dysregulation often leads to limited improvement. By coordinating care and integrating brain based treatment, the focus remained on restoring regulation rather than managing symptoms in isolation. This collaborative approach helped align emotional recovery with neurological healing.
Post Concussion Syndrome Treatment in Tampa: Adjusting Care as mTBI Symptoms Evolve Over Time
Dr. Emily explained that post concussion syndrome treatment must adapt as symptoms change, because recovery is rarely linear. As the brain and nervous system begin to respond, some symptoms improve while others become more noticeable. Ongoing evaluation is essential to understand what the brain needs at each stage of recovery.
In this case, early care focused on identifying both brain dysfunction and spinal injury.
Dr. Gleis, a pain management MD in Tampa, addressed neck and back pain first by prescribing chiropractic care to improve mobility and reduce mechanical stress on the spine. As that care began to help, it provided valuable information about which symptoms were improving and which required further attention.
Dr. Gleis explained that reducing spinal pain is often a necessary first step. By calming pain and nerve irritation, the overall stress load on the nervous system can decrease, allowing the brain more capacity to recover.
Once the response to chiropractic care was clear, next steps could be considered thoughtfully rather than prematurely.
As recovery progressed, emotional and cognitive symptoms became more apparent. Dr. Emily emphasized that this shift did not indicate a setback, but rather revealed additional areas of neurological strain that needed support. Brain treatment was expanded based on these changes, rather than replaced or restarted.
By adjusting care as symptoms evolved, recovery remained responsive instead of reactive. Rather than waiting for symptoms to worsen or forcing the same approach to continue, treatment decisions were guided by observation, response, and ongoing evaluation. This approach helped maintain progress and supported more stable, long term improvement.
Using TMS and HBOT Treatment in Tampa to Support Brain Recovery After a Concussion
As depressive symptoms and emotional dysregulation became more apparent, Dr. Emily explained that additional brain rehab support was needed.
These symptoms were understood as part of the neurological recovery process rather than a separate mental health issue. Based on how the brain was responding, treatment was expanded to support regulation, energy, and recovery capacity.
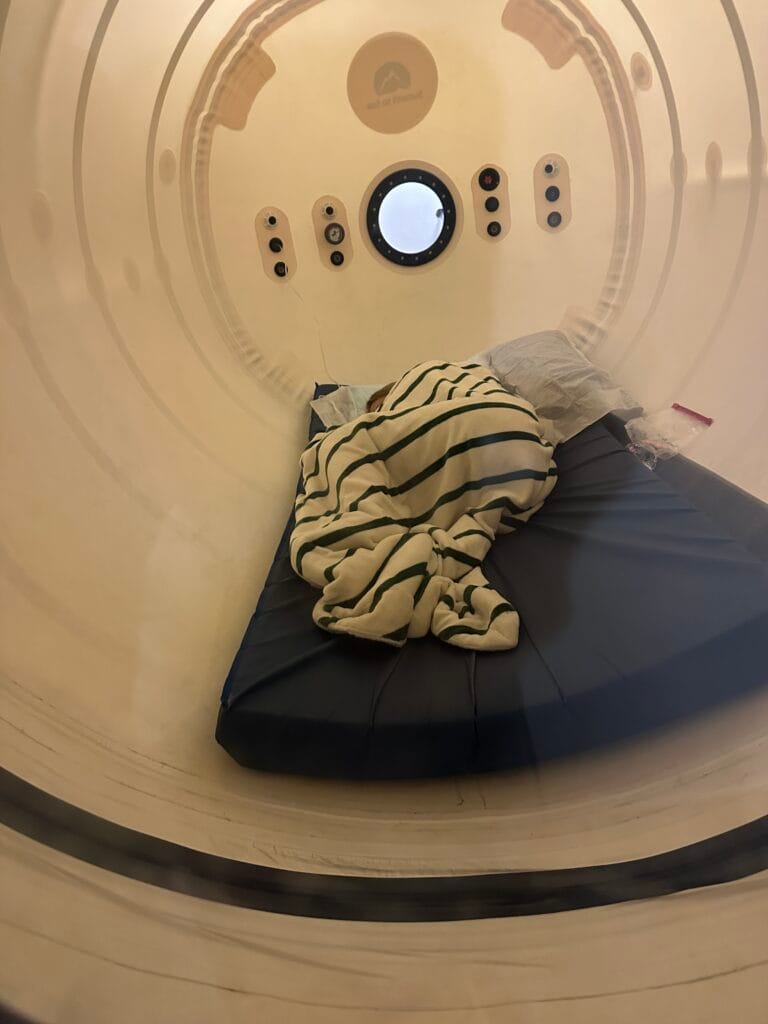
Following Dr. Emily’s referral, the patient was evaluated by Dr. Craig Jorden Jr., who works within the clinic to support patients with neurological and mood related symptoms.
After assessment, Transcranial Magnetic Stimulation was prescribed as a non medication option to support mood regulation and brain function. TMS was selected to help stimulate specific brain regions affected by concussion and ongoing stress.
At the same time, Dr. Emily recommended additional Hyperbaric Oxygen Therapy in Tampa to help. She explained that HBOT helps increase oxygen delivery to the brain, supporting metabolic demand and healing during recovery. By improving oxygen availability, the brain is better equipped to respond to therapies such as TMS and to support neuroplastic change.
Dr. Emily emphasized that TMS therapy and HBOT were not used independently. They were prescribed together as part of an integrated approach to support brain function from multiple angles. TMS helped activate and regulate targeted brain regions, while HBOT supported the underlying physiological environment needed for recovery.
By combining these therapies at the appropriate stage, treatment remained aligned with how the brain was functioning in real time. This coordinated approach helped improve mood regulation, stress tolerance, and overall recovery capacity. Most importantly, it allowed care to continue progressing without relying on medication alone.
Why Additional HBOT Sessions Were Prescribed After TMS Was Added
Hyperbaric Oxygen Therapy was already part of the patient’s care before Transcranial Magnetic Stimulation was introduced.
Dr. Emily explained that HBOT was being used to support brain recovery by improving oxygen delivery during a period of increased neurological demand. As neuro treatment progressed, the patient’s response provided important information about what the brain needed next.
After TMS was added by Dr. Craig Jorden Jr. to support mood regulation and brain activation, Dr. Emily recommended additional HBOT sessions. She explained that as brain activity increases through stimulation, metabolic demand also rises. Providing additional oxygen support helps the brain better tolerate and respond to that increased workload.
Dr. Emily emphasized that this sequencing was intentional. TMS helped activate and regulate specific brain regions to help with the patients depression, while additional HBOT sessions were prescribed to support the brain’s energy needs during that phase of recovery. Rather than introducing treatments randomly, care was adjusted based on how the brain was responding in real time.
By expanding HBOT after TMS was initiated, treatment remained aligned with the brain’s changing needs. This approach helped support recovery without overwhelming the nervous system. It also reinforced the importance of monitoring response and adjusting care, rather than assuming one phase of treatment is sufficient for the entire recovery process.
Measuring Progress With Pre and Post Concussion Evaluations
Dr. Emily explained that progress after a concussion cannot be measured by symptoms alone. While patient experience is important, symptoms often fluctuate during recovery and do not always reflect how the brain is functioning. This is why pre and post concussion evaluations are used to create objective reference points over time.
In this case, qEEG brain mapping was used as part of the evaluation process to assess brain function and nervous system regulation. The initial qEEG established a baseline that helped explain the patient’s symptoms and identified areas of dysregulation following the auto accident in Odessa Florida. This baseline made it possible to track meaningful change rather than rely on guesswork.
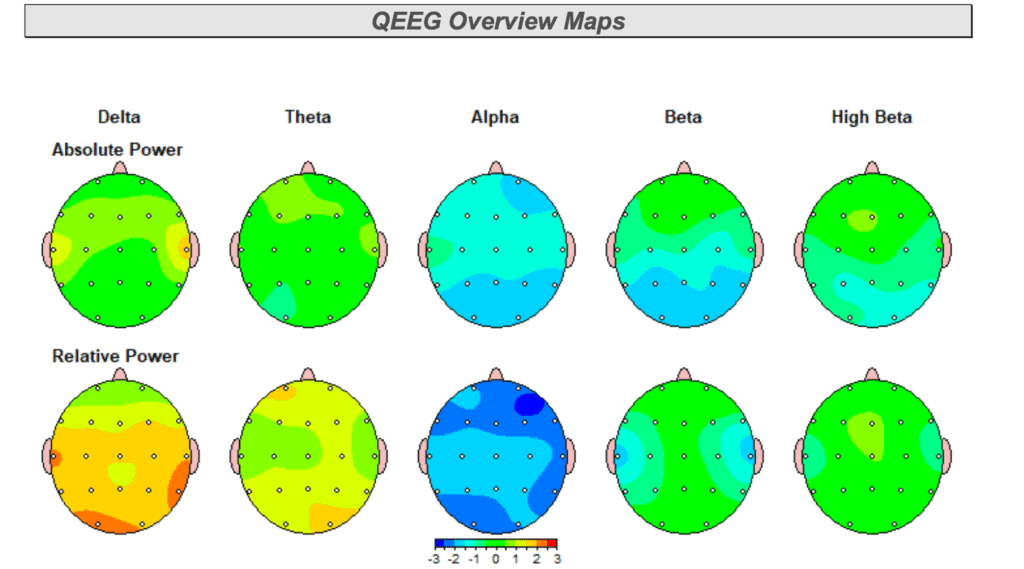
Dr. Emily emphasized that post evaluations are just as important as the initial assessment. As treatments such as chiropractic care, TMS, and additional HBOT were introduced, follow-up qEEG brain mapping in our Tampa office helped confirm how the brain was responding. This ensured that care remained aligned with recovery rather than continuing unchanged.
Pre and post concussion evaluations also helped explain why recovery did not follow a straight line. Some symptoms improved quickly, while others appeared later as the brain adapted and demands increased. Having measurable data helped validate the patient’s experience and reduced uncertainty during periods of change.
Most importantly, these evaluations supported informed decision making. Instead of guessing when to add, pause, or adjust treatment, care was guided by documented changes in brain function and regulation. This approach helped maintain momentum and reinforced that recovery was occurring, even when progress felt uneven.
A Multidisciplinary Treatment Plan for Post Concussion Syndrome Recovery
Dr. Emily emphasized that post concussion syndrome recovery rarely depends on a single therapy. Because brain function, spinal injury, mood regulation, and nervous system stress are interconnected, treatment must address multiple systems at the same time. For this reason, care was structured as a coordinated plan rather than isolated interventions.
In this case, treatment included care for both spinal injury and brain function. Chiropractic care was used to improve mobility and reduce mechanical stress on the nervous system. As pain decreased, the brain had more capacity to regulate and respond to neurological therapies.

Neuro rehabilitation therapies were layered in to support brain and nervous system regulation. Neurofeedback was used to help the brain move toward more stable and efficient activity patterns. Biofeedback and vagus nerve focused therapies were incorporated to support autonomic regulation, helping the nervous system shift out of a prolonged stress state following the accident.
Light based therapy was also used as part of the neuro rehabilitation process. Dr. Emily explained that light therapy can support brain activation and regulation, particularly when the nervous system has been under sustained strain. This therapy was used to complement other treatments rather than replace them.
As recovery progressed, brain based therapies were adjusted based on response. The qEEG brain map guided care helped identify areas of dysregulation, Transcranial Magnetic Stimulation supported mood and brain activation, and Hyperbaric Oxygen Therapy was used throughout treatment and expanded as needed to support oxygen delivery and metabolic demand. Each therapy served a distinct purpose within the broader plan.
Dr. Emily explained that this approach allows treatments to work together rather than compete. Some therapies reduced stress on the nervous system, while others supported activation, regulation, or recovery capacity.
When combined intentionally, they created a more stable environment for neurological recovery without relying on medication.
This multidisciplinary treatment plan allowed care to evolve with the patient. By addressing physical pain, brain function, nervous system regulation, and mood together, recovery stayed aligned with how the brain was responding in real time. This coordination helped prevent stalls in progress and supported more consistent improvement.
What This mTBI Case Teaches Patients and Families After a Car Accident
One of the most important lessons from this case is that not all injuries are immediately obvious. After a car accident, symptoms can evolve over time as the brain, spine, and nervous system respond to stress and trauma. Waiting for clarity can sometimes delay the very care that helps prevent long term complications.
This case also highlights why getting checked out early matters, even when uncertainty exists. Objective evaluations such as qEEG brain mapping, balance testing, and clinical interviews helped identify areas of strain before symptoms became overwhelming. That early documentation created a foundation for treatment decisions and protected against confusion later in the recovery process.
Another key takeaway is that recovery often requires addressing more than one system at a time. Treating spinal pain alone or focusing only on mood would not have been sufficient. By evaluating brain function, nervous system regulation, and physical injury together, care could be adjusted as new symptoms emerged rather than starting over each time something changed.
Finally, this case underscores the value of coordinated care. When clinicians communicate and treatments are layered intentionally, recovery becomes more organized and less reactive. That structure helps patients and families feel supported during a process that can otherwise feel unpredictable.
Hope After Post Concussion Syndrome Treatment
Post concussion syndrome can feel discouraging, especially when symptoms linger or change over time. Many patients begin to wonder whether what they are experiencing is permanent or whether improvement is still possible. This case shows that progress can occur when care is guided by objective information and adjusted thoughtfully.
Hope does not come from ignoring symptoms or pushing through them. It comes from understanding what the brain and nervous system need at each stage of recovery. Through ongoing evaluation, targeted therapies, and coordinated care, improvement can be supported even when the path is not linear.
At Genesis Brain Institute, cases like this reinforce an important principle: every brain is different, and recovery should reflect that. When brain treatment is individualized and progress is measured over time, patients are no longer left guessing whether they are getting better.
Most importantly, this story reminds patients and families that feeling “off” after an accident is worth paying attention to. Getting checked out early can provide answers, direction, and reassurance. With the right support, post concussion syndrome does not have to define the future, and healing can continue well beyond the initial injury.
Next Step to Get Checked Out after an Auto Accident In Tampa
If you want to understand how your brain is functioning through the Quant360 Functional Analysis schedule a consultation or request more information at GenesisBrainInstitute.com. Every brain deserves to feel calm, confident, and connected again, especially if you’re suffered a TBI after a car accident.
Disclaimer: This content is for informational purposes only and does not constitute medical advice. Please consult with a licensed healthcare provider. Genesis Brain Institute is a Brain Treatment Center in Tampa offering non-pharmaceutical solutions that bring clarity, restore function, and offer real hope for those who feel lost, stuck, or simply want more from life.